Every so often you may come across a news headline about how much something impacts your risk of cancer and it makes you pause. Take for instance a headline, “Heavy Alcohol Drinking Increases the Chances of Getting Oral Cancer Fivefold.” Now you are wondering what this means and what your likelihood of getting cancer is. You may dive into the story or even dig up the study it was based on looking for clarity, only to become more confused by jargon—rate ratio, hazard ratio, relative risk, baseline risk, or absolute risk.
Elizabeth A. Platz, ScD, MPH, an epidemiology professor and researcher from Johns Hopkins Bloomberg School of Public Health and the Sidney Kimmel Comprehensive Cancer Center, understands how these concepts can be confusing for the general public—and perhaps even a little deceiving.
“Many considerations go into calculating and interpreting these risk estimates, so it can be hard for the public to understand what these numbers really mean without the full picture,” said Platz, who is the editor-in-chief of the American Association for Cancer Research (AACR) journal Cancer Epidemiology, Biomarkers & Prevention. “For example, it is important to consider what is the risk of cancer if someone doesn’t have the exposure, how many people have the exposure, is the study only looking at a specific subset of the population, and if there are any other factors that are associated with the exposure and with the cancer.”
To offer some clarity, Platz provided simplified explanations behind how cancer risks are studied, the concepts that go into cancer risk estimates, and how to better interpret what the numbers mean.
How Are Cancer Risk Factors Studied?
Cancer epidemiologists like Platz study the occurrence and potential causes of cancer in a defined population. First, they ask a research question about a potential cause and then form a hypothesis they want to test. Those potential causes are often referred to as “factors,” which may be inherited conditions or exposures to something in our environment. They could also be modifiable factors—which are known to cause about 40% of cancer cases in the United States—such as smoking, excess body weight, alcohol, ultraviolet radiation, poor diet, and physical inactivity.
Often, these studies are observational, in which participants are observed in their natural settings, and the researcher does not directly intervene to change who is and is not exposed to the factor. In other cases, the researchers can identify a group of people who have cancer, determine who was exposed to the factor and who wasn’t, and do a retrospective analysis of the effect of that factor.
The chances that anyone gets cancer is binary—they either get it or they don’t. What risk inherently looks at is the number of events—in this case the people who get cancer—divided by the number of people at risk for that event.
Platz explained that the larger the study the better, as more participants result in more precise estimates. Meta-analyses, in which results from multiple studies that have already been conducted are combined, or consortium studies, where researchers pool the data from the studies that they are each conducting, provide even more precise estimates.
But one aspect of epidemiologic studies that Platz wanted to make clear is that they examine risk at a population level.
“Risk is not an individual-level concept,” Platz said. “The chances that anyone gets cancer is binary—they either get it or they don’t. What risk inherently looks at is the number of events—in this case the people who get cancer—divided by the number of people at risk for that event.”
When a doctor is telling a patient their likelihood of getting a disease such as cancer, Platz explained, the doctor is doing so based on what large studies found about people who share similar characteristics to them such as age, sex, weight, smoking history, family history, and other risk factors. For that reason, a person’s risk will vary depending on how closely their characteristics match those in the study population.
Calculating Cancer Risk and Relative Risk Estimates
Researchers take what they have learned from large studies to calculate risk estimates. These are considered estimates because the researchers are only studying a sample of the entire population at risk.
When presenting these results, Platz explained, epidemiologists will talk about “relative risk,” which can refer to specific measurements like the “rate ratio” or “hazard ratio.” But fundamentally, any relative risk estimate is trying to get at the same idea: how much higher the likelihood of cancer in one group is compared with another group. Additionally, researchers may look at “absolute risk”—or simply, risk. In this case, risk is not calculated in comparison to another group.
To help nonexperts better understand the various calculations behind these estimates, Platz offered the following explanations.
Incidence Rate
Incidence rate is the number of people in a group who got cancer divided by the sum of time everyone in the group was followed while they were at risk (this is often called person-time or person-years at risk by researchers).
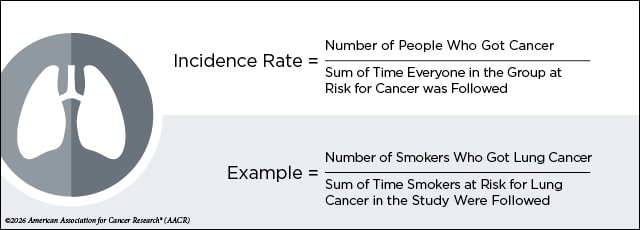

For example, if a person was followed for all 10 years in a study and they never were diagnosed with cancer, remained alive, and were still in the study, then they contribute a total of 10 years to the sum. If they were only followed for three months, then they contribute a total value of 0.25 years to the sum.
Rate Ratio
The rate ratio—or more specifically, the incidence rate ratio—is the incidence rate of cancer in people who are exposed to the factor being studied compared with the incidence rate of cancer in people who are not exposed.
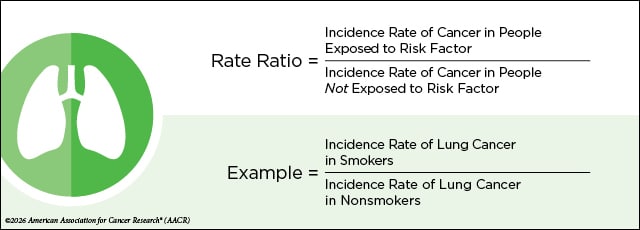
Exposures with rate ratios consistently greater than 1 are called risk factors, while exposures with rate ratios consistently lower than 1 are called protective factors. When the rate ratio is equal to 1, the exposure is not associated with cancer risk.
Hazard Ratio
The difference between hazard ratio and rate ratio is how time is factored in using instantaneous rate. Instantaneous means, Platz explained, at any given moment during which the at-risk participants are followed for a first cancer diagnosis. The hazard ratio then compares the instantaneous rate of cancer in those who are exposed to a risk factor to the instantaneous rate of cancer in those who are not exposed.
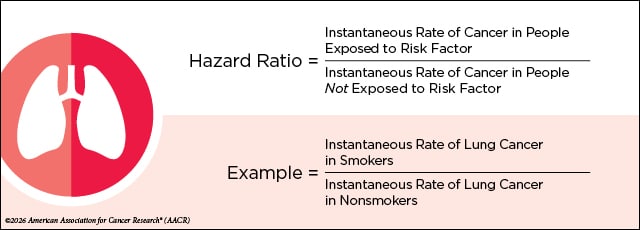

Similar to rate ratio, anything less than or greater than 1 would indicate that an exposure is a protective factor or a risk factor, respectively.
Absolute Risk
In a basic sense, absolute risk is the rate of people exposed to a risk factor who got cancer over a set period. For example, the absolute risk for smoking and lung cancer would look at how many smokers got lung cancer divided by the number of smokers at risk for lung cancer during a specific timeframe. Time is crucial because while the risk of death over a lifetime is 100%, it is not 100% over the next minute or year.
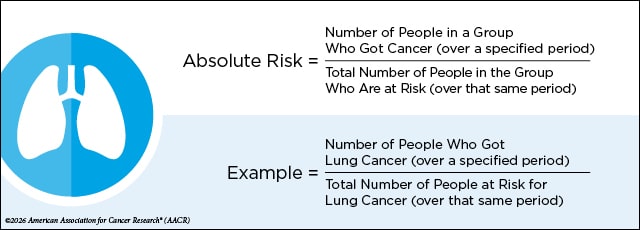
In actual studies, the calculation of absolute risk is a bit more complicated as it takes into account that some participants may stop participating or die during the study.
Additionally, papers may mention different subtypes of absolute risk, such as:
- Baseline risk: This is the risk of cancer in people prior to being exposed to a risk factor. Once a person is exposed to a risk factor, the baseline risk can be used to determine how much their chances of cancer have changed.
- Lifetime risk: This calculation takes several factors into consideration to estimate how likely a person who is free from cancer at birth will develop cancer during some point in their life.
“Some people may hear the lifetime risk of cancer for men is 1 in 2 and think that means half of their male friends will be diagnosed with cancer in the next five years,” Platz said. “But that estimate covers from birth to an advanced age like 90+ years old or to the typical life expectancy in a population.”
Some people may hear the lifetime risk of cancer for men is 1 in 2 and think that means half of their male friends will be diagnosed with cancer in the next five years. But that estimate covers from birth to an advanced age like 90+ years old or to the typical life expectancy in a population.
Understanding What the Risk Estimate Numbers Mean
To better understand what a relative risk estimate really means, Platz said to imagine two hypothetical studies about the impact of heavy alcohol consumption on cancer risk.
In one study, heavy drinkers compared with light drinkers were found to have a 5 times greater risk of “cancer type x,” while in another study heavy drinking was associated with a 1.6 greater risk of “cancer type y.”
Another way that you may see these estimates interpreted is that heavy drinkers have a 400% higher risk of “cancer type x” and a 60% higher risk of “cancer type y” compared with those who don’t drink or only occasionally drink.
“In both cases, heavy drinking will increase the chances of getting these cancers, but without factoring in absolute risk, you can’t really understand the impact of these relative risk estimates on the population,” Platz said.
Some cancers are rare, while some cancers are more common in a population. So, in this hypothetical, if the baseline risk of “cancer type x” is 0.5% over the lifetime and the baseline risk of “cancer type y” is 13% over the lifetime, even though the relative risk for heavy drinkers is higher for “cancer type x,” the baseline risk will only increase by an absolute 2% to 2.5% compared with an absolute increase of 7.8% to 20.8% for “cancer type y.”
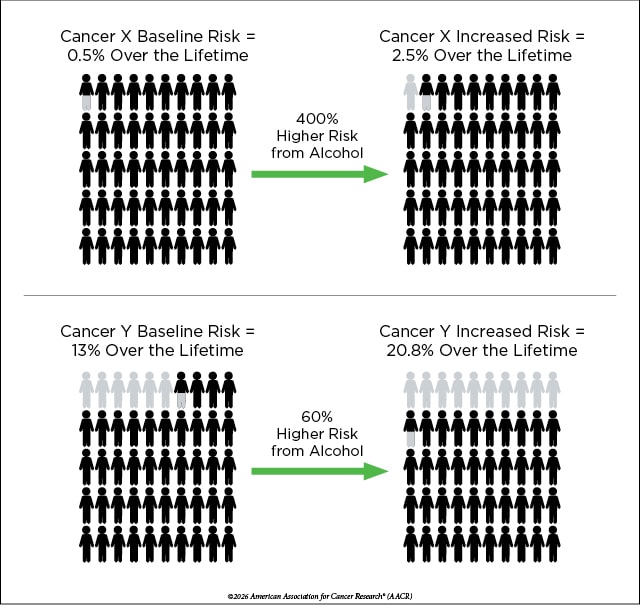
“If the baseline risk is small, then even a relative risk that seems like a huge increase may only result in a small increase in cancer cases,” Platz explained. “Meanwhile, what may appear to be a small relative risk increase could lead to many more cases if the baseline risk is already high.”
Additionally, the prevalence of exposure to a risk factor will also determine how many people are ultimately impacted. As an example, Platz cites outdoor air pollution, which is classified by the International Agency for Research on Cancer (IARC) as carcinogenic to humans, in particular for lung cancer. Even if the particulates in air pollution may be linked to a small increase in the risk of getting a disease, when a large population is exposed to air pollution, it translates to a lot of people having an increased risk of that disease.
What Other Factors Are Considered in Cancer Risk Estimates?
Risk can also vary by cancer type for different populations. For instance, cancer incidence is generally higher in older individuals, so their risk even when not exposed to risk factors is already higher than younger individuals. Additionally, some cancers are more common in certain races and ethnicities or genders. So, when looking at how cancer risk estimates might pertain to you, Platz suggests examining what populations were included in the study.
Additionally, more than one modifiable risk factor could contribute to the development of cancer, which researchers take into account by considering confounding variables and effect modification. A confounding variable is when a risk factor may distort the association with cancer of another risk factor, if researchers do not adjust for it. Effect modification is when two risk factors may interact with each other to further exacerbate the chances of cancer or another disease.
People sometimes think if they go to the gym or go for a walk, that’s good enough, but this study showed that if you’re sitting the rest of the time then it’s not. These are the types of insights researchers look for when they study the size of associations between various risk factors.
As an example of effect modification related to mortality, Platz pointed to a 2020 meta-analysis on physical activity and sedentary time in which researchers wanted to better understand if a certain amount of physical activity could cancel the effects from too much sedentary time, which is associated with higher risks of mortality. The researchers examined data from 44,370 individuals and found that even if individuals engaged in the recommended amount of physical activity each week, greater sedentary time was still associated with a higher risk of death.
“People sometimes think if they go to the gym or go for a walk, that’s good enough, but this study showed that if you’re sitting the rest of the time then it’s not,” Platz explained. “These are the types of insights researchers look for when they study the size of associations between various risk factors.”
