Fatty liver disease not caused by alcohol is quickly emerging as a major public health concern in the United States.1 It often develops silently over many years, with contributors like obesity, Type 2 diabetes, and insulin resistance. Symptoms — such as a swollen belly, unexplained weight loss, extreme fatigue, and pain in the upper right abdomen — usually don’t show up until the condition has progressed.2
But even if it’s advanced, it’s not too late. Fatty liver is a reversible condition, and addressing it can lead to real improvements in your health.
Many doctors will recommend GLP-1 agonists like Ozempic for patients with liver disease, especially when there is co-existing obesity or Type 2 diabetes.3 However, there are many downsides to this approach, such as poor mental health, lower bone and muscle density, and a host of digestive issues. Worse, you can rebound from Ozempic, which means you’ll regain the weight you’ve lost once you stop taking the drug.4
The good news is there are far safer, healthier alternatives. The most important remedy for fatty liver disease is choline, as your body simply cannot get rid of liver fat without it, and choline deficiency is rampant (We’ll get back to that later). Researchers are also looking into niacin for fatty liver disease treatment, and while the results are promising, this is an incomplete picture — niacinamide is the better alternative, which I’ll also explain below.
Where Niacin Fits Into the Picture of Fatty Liver Disease
In a study published in Metabolism, researchers from Korea discovered the role of microRNA-93 (miR-93) in attenuating fatty liver disease.5 For context, miR-93 is a unique ribonucleic acid (RNA) that helps suppress the expression of certain genes. To perform the experiment, the team used transcriptome analysis, allowing them to identify how the process unfolded.
They also used a screening system to test drugs that can modulate miR-93 expression, particularly niacin. A preprint of the study sheds further light on these findings:6
• At the center of the findings sits miR-93 — Micro RNAs act like molecular messengers inside cells. They do not build proteins themselves. Instead, they tell cells which instructions to ignore. In this study, miR-93 blocked a protein called SIRT1, which plays a central role in cellular energy regulation. When miR-93 levels rose, SIRT1 activity dropped, and liver metabolism shifted toward fat storage rather than fat use.
The researchers showed that when miR-93 rose, liver cells lost control over a major energy pathway known as the LKB1-AMPK system. When energy runs low, AMPK pushes cells to burn fat and restore balance. Suppressing SIRT1 shuts that system down. As a result, fat piled up in liver cells, mitochondria slowed, and metabolic stress increased.
• Animal data strengthened the hypothesis — Mice engineered to lack miR-93 resisted fatty liver even when fed a high-fat diet. These mice also had lower liver fat, less inflammation, improved insulin sensitivity, and stronger mitochondrial activity. In contrast, normal mice with elevated miR-93 developed classic fatty liver features.
• How niacin enters the picture — The authors reported that niacin treatment suppressed miR-93 expression in liver tissue. When miR-93 levels fell, SIRT1 activity rebounded. That rebound restored AMPK signaling and improved fat handling inside liver cells. In both human liver samples and mouse models, niacin reversed the molecular fingerprint tied to fatty liver disease.
• AMPK sits downstream of SIRT1 and amplifies the effect — When AMPK remains active, liver cells burn fat, regulate glucose, and maintain insulin sensitivity. When AMPK shuts down, fat accumulates and metabolic chaos follows. The study showed that niacin restored this pathway, starting at miR-93 suppression and ending with improved mitochondrial output.
Another important finding involves the mitochondria themselves. The researchers linked high miR-93 levels to impaired mitochondrial respiration. When they falter, the liver shifts into fat storage mode. Niacin restored mitochondrial efficiency by reopening the SIRT1-AMPK pathway, allowing liver cells to generate energy instead of hoarding fat.
Does Niacin Improve Liver Fat or Enzymes?
The Metabolism study isn’t the only published research to make the connection between niacin and improved liver fat turnover. In a 2024 study published in JAMA Network Open, researchers investigated a similar angle — the role of dietary niacin intake on long-term survival of people diagnosed with fatty liver disease.7
A total of 4,315 people aged 20 and older with fatty liver disease were selected using data from the National Health and Nutrition Examination Survey (NHANES), which was conducted between 2003 and 2018. Over a median follow-up of 8.8 years, 566 participants died from any cause and 197 died from cardiovascular causes.
• Participants who ingested more niacin had better mortality odds — Those who had the highest dietary niacin intake showed a significantly lower risk of death from all causes compared with those with the lowest intake.
Specifically, participants consuming 26.7 milligrams (mg) of niacin per day or more had a 30% lower risk of all-cause mortality than those consuming 18.4 mg per day or less, even after adjusting for age, sex, body mass index, smoking, alcohol intake, physical activity, and overall diet quality.
• Consistency played an important role — The survival advantage emerged over nearly a decade of follow-up. This suggests niacin intake supports long-term metabolic stability rather than producing short-lived effects.
• The research showed niacin’s role in nicotinamide adenine dinucleotide (NAD+) metabolism — It acts as a central cofactor in cellular energy production, DNA repair, and mitochondrial function. When NAD+ availability declines, cells struggle to produce energy efficiently. In fatty liver disease, this energy deficit drives cellular stress and systemic dysfunction.
Higher niacin intake supports NAD+ synthesis. More NAD+ improves mitochondrial efficiency, enhances oxidative metabolism, and stabilizes cellular stress responses.
• Another study reinforces the benefits of niacin — In a study published in Therapeutic Advances in Chronic disease,8 researchers investigated how nicotinamide (a different form of niacin9) can help improve fatty liver disease and overall metabolic health.
Alanine aminotransferase, a liver enzyme that rises when liver cells sustain injury, dropped by an average of 26.6% in the nicotinamide group compared with 0.74% in the control group over the same period.
• Beyond liver enzymes, lipid markers improved — Participants receiving nicotinamide showed statistically significant reductions in total cholesterol and low-density lipoprotein (LDL) cholesterol compared with controls. These changes matter because dyslipidemia accelerates fatty liver progression and cardiovascular risk among diabetics. Improving lipid balance reduces the metabolic pressure that feeds liver dysfunction.
• Insulin resistance also improved — The nicotinamide group demonstrated a significant reduction in insulin resistance indices compared to the control group by week 12. Insulin resistance drives fat accumulation in the liver and worsens glycemic control. Improving this marker directly supports better glucose handling and metabolic stability.
The Ideal Niacin Dosage for Fatty Liver Disease
Now that you’re familiar with the importance of niacin, the next step is figuring out the optimal intake amount, as the featured studies showcased different doses. For example, the researchers from the Metabolism study administered 200 mg per kilogram (kg) of weight in test mice.10 In the JAMA Network Open study, 26.7 mg produced health benefits, but this was only an average intake — not a definite dosing recommendation.11
For better guidance, the recommended dietary allowance for niacin is listed below. These dosages are what the Office of Dietary Supplements recommends for healthy individuals; if you’re deficient, you likely need more:12
| Age | Male | Female | Pregnancy | Lactation |
|---|---|---|---|---|
| Birth to 6 months | 2 mg | 2 mg | ||
| 7 to 12 months | 4 mg | 4 mg | ||
| 1 to 3 years | 6 mg | 6 mg | ||
| 4 to 8 years | 8 mg | 8 mg | ||
| 9 to 13 years | 12 mg | 12 mg | ||
| 14 to 18 years | 16 mg | 14 mg | 18 mg | 17 mg |
| 19 years and above | 16 mg | 14 mg | 18 mg | 17 mg |
• Recommended niacin formulations — Due to the various niacin supplements out in the market, it can get confusing from the viewpoint of consumers. Look for “timed release” preparations, as well as similar terms such as controlled release, slow release, sustained release, prolonged release, and long-acting niacin.13 That said, there’s ample reason to opt for niacinamide instead of niacin, as I’ll explain in the next section.
• Top food sources of niacin — While supplementation has been shown to help, it’s not the only option available — you can also get it from your diet. Some of the foods with the highest amounts of niacin include grass fed beef liver, chicken breast (make sure to look for pastured organic chickens), wild-caught sockeye salmon, and potatoes.14
Why Niacinamide Is the Superior Choice Compared to Niacin
Where does niacinamide enter the picture, you may wonder? While it sounds like niacin (and the two are often erroneously interchanged), this is where the similarities end. To set the record straight, I generally recommend niacinamide over niacin because it’s the best NAD+ precursor, as the immediate breakdown product of NAD+ is niacinamide.
• NAD+ is a key molecule that fuels energy production in your mitochondria — When NAD+ levels become low, your cells won’t be able to convert the food you eat into energy, which forces your body to break down muscle tissue to survive — not an ideal situation.
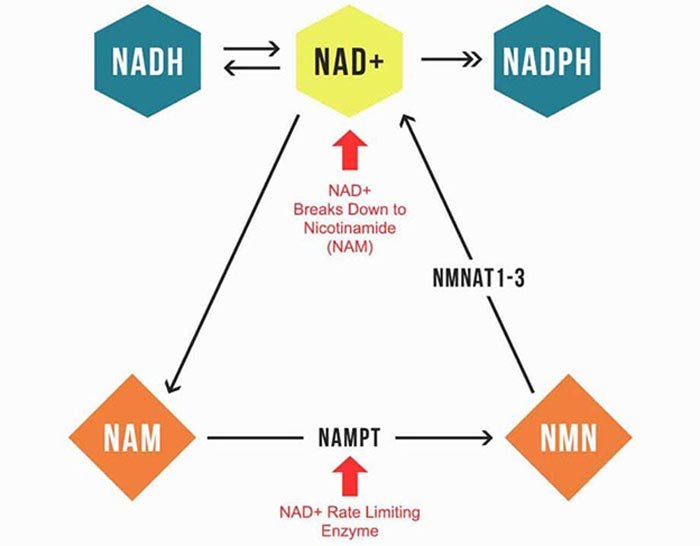
Next, when NAD is used up, it gets broken down into niacinamide (also known as nicotinamide), which is recycled. It’s converted into nicotinamide mononucleotide (NMN), and then back into NAD+. The process is outlined in the image below.
• Dosing recommendation of niacinamide — For optimal results, I recommend taking 50 mg of niacinamide three times a day. In addition to being a more direct way to increase NAD+, niacinamide is also far more cost-effective — it will only cost you $25 a month if you get it as a powder.
• Niacinamide powder is the optimal form to take — Generally, a 1/64 teaspoon of niacinamide powder is around 50 mg. For your convenience, you can easily buy a measuring set on amazon that contains a 1/64 teaspoon.
Now, the reason why I recommend it in powder form is because you can easily control your intake. Most supplements brands set the lowest dose at 500 mg, which isn’t ideal — this high a dose actually decreases NAD+ due to negative feedback on NAMPT, the rate-limiting enzyme for NAD+, which controls the amount of NAD+ your body produces.
• Niacinamide doesn’t cause skin flushing — Both niacin and niacinamide are forms of vitamin B3, and in the context of typical low-supplement dosages, they are routinely considered interchangeable. However, niacin causes flushing, which is a temporary side effect wherein the blood vessels become dilated, causing the skin to become more redder or pinker than usual. Niacinamide does not cause this.
Key Risks to Discuss with Your Doctor
While the studies show that niacin offers important benefits, it’s essential to be aware of the possible risks, especially at higher doses or when combined with certain medications. Discuss the following concerns with your healthcare provider:
• Liver injury — High-dose (or extended release) niacin has caused clinically significant hepatotoxicity, including severe cases. Risk rises with sustained-release forms, dose escalation, and self-medication without monitoring. If any of these apply to you, stop immediately and seek care for possible jaundice, dark urine, severe fatigue, or itchy skin.15
• Glycemia and insulin resistance — High-dose niacin can worsen glucose tolerance in some patients. Intensify glucose monitoring if used.16
• Uric acid and gout — Niacin can raise uric acid and precipitate gout flareups among susceptible individuals.17
• Drug combinations — There are certain medications that can interfere with niacin supplementation. For example, isoniazid and pyrazinamide (tuberculosis medications) hamper niacin production from tryptophan. Moreover, isoniazid can inhibit NAD production.18
Choline — A Cornerstone of Fatty Liver Management
While your liver may benefit from niacinamide, increasing choline intake is a far better foundational strategy. That’s because choline is required to transport fat out of the liver.
Your liver produces very low-density lipoprotein (VLDL), which transports triglycerides and some cholesterol from your liver to other tissues. VLDL assembly requires phosphatidylcholine, which depends on adequate choline availability. When hepatic (liver) choline/phosphatidylcholine is too low, VLDL secretion is impaired, so triglycerides are less efficiently exported and accumulate in liver cells, resulting in fatty liver disease.
• Food is the best source of choline — Egg yolks (especially pastured ones) are the richest and safest way to meet your choline needs. Other sources include organic muscle meats and wild-caught fish, which provide moderate amounts.
Vegetables that contain small amounts of choline include cruciferous vegetables, such as broccoli, cauliflower, and Brussels sprouts. For those who follow a plant-based diet, you’ll likely need to take a supplement to support your liver health, as you simply cannot eat enough vegetables to meet the needs of your liver.
• Take a choline supplement if diet alone isn’t enough — There are several choline supplements available on the market, but the only one I recommend is citicoline, primarily due to its superior bioavailability
• Recommended intake — Your choline intake will depend on your age. For example, adult men generally need 550 mg of choline per day, while adult women need 425 mg per day. Infants will need 125 to 150 mg per day while children (around 4 to 8 years old) will need 250 mg per day. Use this as a guide to know if you’re getting enough.
For a more in-depth understanding of how choline provides a vital line of defense for your liver, see “A Mortal Enemy of Your Liver, It’s Not Alcohol.”
Other Tips to Help Protect Your Liver from Further Damage
While the findings regarding niacin show promise, don’t rely on it alone to manage fatty liver disease. It would be wise to follow a holistic approach, as this can maximize your outcomes. Here are other strategies I recommend you follow:
1. Eliminate vegetable oils and alcohol right away — If your diet includes packaged or restaurant foods made with soybean, canola, corn, sunflower, or other vegetable oils, your liver is taking a nonstop hit. These oils are high in linoleic acid (LA), a fragile polyunsaturated fat (PUF) that drives fat accumulation in the liver and fuels oxidative damage.
Your body converts LA into oxidized linoleic acid metabolites (OXLAMs), which are unstable compounds that harm mitochondria and interfere with cellular energy production.
To protect your health, keep your LA intake to below 5 grams a day, but if you can keep it to below 2 grams, that’s even better. For better monitoring, sign up for the Mercola Health Coach app once it becomes available. It will contain the Seed Oil Sleuth, a feature that can help monitor the LA in your food to a tenth of a gram. In addition, use healthy fats like grass fed butter, ghee, tallow, or coconut oil when cooking your food.
Alcohol also compounds the problem. When metabolized, it becomes acetaldehyde, a toxic byproduct that damages liver cells from the inside out. If you’re already showing signs of fatty liver or insulin resistance, removing both vegetable oils and alcohol is one of the fastest ways to give your liver a chance to heal.
2. Move daily and focus on reducing waist size — There’s no need for intense workouts or long gym sessions. A 10- to 20-minute brisk walk after meals, daily stretching, and a couple of weekly strength or bodyweight sessions are enough to make a difference.
Regular movement lowers insulin levels and improves blood flow and oxygen delivery to the liver. A waist circumference over 40 inches for men or 35 inches for women signals excess visceral fat, which is strongly associated with liver fibrosis.
3. Make high-quality sleep a priority to calm inflammation — Poor and/or insufficient sleep robs your liver of the recovery time it needs. Aim for deep, uninterrupted rest in a dark, cool environment.
Stop eating at least three hours before sleeping to avoid nighttime blood sugar disruptions. Even modest improvements in sleep quality can lower inflammation and gradually improve insulin sensitivity, easing the burden on your liver. For additional information, read “Subtle Signs You Are Not Getting Enough Sleep.”
Frequently Asked Questions (FAQs) About the Link Between Niacin and Fatty Liver Disease
Q: Does niacin help with fatty liver disease?
A: Yes. Research shows niacin can improve fatty liver by restoring key metabolic pathways that promote fat-burning instead of fat storage. Higher dietary niacin intake has also been linked to better long-term outcomes in people with fatty liver disease.
Q: Is niacin safe if I already have fatty liver?
A: It can be safe at low to moderate intakes, especially from food. High-dose niacin, particularly without supervision, can stress the liver. Anyone with fatty liver disease is advised to use niacin only with medical guidance and monitoring.
Q: What dose of niacin is used for fatty liver?
A: There is no established treatment dose. Benefits have been seen at dietary intakes around 26.7 mg per day. Higher supplemental doses raise safety concerns and should only be used under medical supervision.
Q: Does niacin worsen blood sugar or insulin resistance?
A: High doses can worsen blood sugar control in some people. Lower doses and certain forms, such as nicotinamide, have been shown to improve insulin resistance. Monitoring is important if you have diabetes.
Q: What is niacinamide and why is it better than niacin?
A: Niacinamide is a form of vitamin B3 that helps your body produce NAD+, a critical molecule needed for mitochondrial energy production and healthy metabolism. It’s considered better than niacin because it’s a more direct and efficient NAD+ precursor, is easier to dose in smaller amounts, and does not cause the uncomfortable skin flushing that niacin often triggers. It is also generally better tolerated, whereas high-dose niacin can carry greater risks like liver strain.
Q: Why is choline important for the management of fatty liver disease?
A: Your liver produces very low-density lipoprotein, or VLDL, which transports triglycerides and some cholesterol from your liver to other tissues. When choline intake falls too low, your liver cannot package and export fat efficiently, so triglycerides remain in liver cells and accumulate over time, resulting in fatty liver disease. To boost intake, food sources are the best, such as egg yolks, organic muscle meats, and wild-caught fish.
Test Your Knowledge with Today’s Quiz!
Take today’s quiz to see how much you’ve learned from yesterday’s Mercola.com article.
What portion of global deaths is linked to cardiovascular disease?