Respiratory infections remain the stealth threat that transforms independent older adults into hospital patients who don’t always recover. What’s becoming impossible to ignore: these outcomes often trace back to a single, correctable biological vulnerability, not bad luck or inevitable exposure.
Large population data now place vitamin D status squarely in that conversation, not as a background nutrient but as a defining factor in how well your respiratory system holds its ground under stress. Unlike vitamins that simply fill nutritional gaps, vitamin D acts as a hormone — a chemical messenger that travels through your bloodstream, instructing cells throughout your body how to respond to threats.
It essentially reprograms your immune system’s response to infection. Because your body is designed to make it via sunlight exposure, deficiency often develops in people who spend more time indoors, live at northern latitudes, or carry metabolic strain that interferes with normal processing.
Deficiency symptoms masquerade as everyday complaints — another cold, lingering fatigue, slower healing — until a serious respiratory infection reveals what’s been deteriorating invisibly for months or years. What stands out in large-scale data is how consistently vitamin D status correlates with respiratory outcomes, regardless of age, ethnicity, or existing health conditions.
The consistency of those findings reframes vitamin D deficiency as a systems-level problem affecting immune readiness where it matters most: your lungs and airways. From there, the question becomes less about whether vitamin D matters and more about what happens when levels fall far enough to cross a biological tipping point.
Severe Vitamin D Deficiency Sends More People to the Hospital with Respiratory Infections
A study published in The American Journal of Clinical Nutrition examined whether vitamin D levels predict hospital admissions for respiratory tract infections in adults.1 Researchers evaluated 36,258 people from multiple ethnic groups and age ranges, allowing researchers to test whether vitamin D status mattered broadly or only in specific populations.
• Severe deficiency stood out as the true danger zone — The most striking finding involved people with very low vitamin D levels below about 6 ng/mL (15 nmol/L). Compared with adults whose levels reached at least 30 ng/mL (75 nmol/L), severe deficiency increased hospitalization risk by 33%, meaning 1 in 3 additional hospitalizations could be prevented by correcting this single nutrient deficit.2
• Small increases in vitamin D delivered measurable benefits — When researchers looked at vitamin D as a continuous scale rather than categories, they found a steady pattern.3 For every 4 ng/mL (about 10 nmol/L) increase in blood vitamin D, the risk of hospitalization for respiratory infection dropped by about 4%.
• Immune defense in the lungs explains the connection — Vitamin D supports immune cells that line your respiratory tract and act as first responders against viruses and bacteria. These cells rely on vitamin D to produce antimicrobial peptides — your body’s natural antibiotics that punch holes in viral and bacterial invaders, stopping them before they multiply. Without enough vitamin D, this early defense weakens.
• Inflammation control plays a second role — The study also discussed vitamin D’s role in balancing immune reactions. Adequate levels help prevent excessive inflammation that damages lung tissue during infection. When levels drop too low, inflammation becomes harder to control, increasing the likelihood that a respiratory illness escalates to a hospital-level event.
Higher Vitamin D Levels Improve Survival Following Pneumonia
A separate study published in Open Forum Infectious Diseases examined whether vitamin D status at the time of hospital admission predicted survival after community-acquired pneumonia, a serious lung infection that develops outside hospital settings.4 Researchers followed 514 adults admitted to a Danish hospital system and tracked death rates during hospitalization and for six months afterward.
Many of the participants were older and living with chronic conditions such as heart disease, lung disease, or diabetes. Vitamin D status was measured immediately at admission and grouped as sufficient, insufficient, or deficient. Researchers then compared death rates while accounting for age, smoking, body weight, disease severity, and existing illness burden.
• Vitamin D deficiency sharply increased the odds of dying months later — Patients classified as vitamin D deficient faced a 3.5-fold higher risk of death within 90 days compared with those who had sufficient levels. That elevated risk persisted at 180 days, with deficient patients still showing more than triple the mortality risk.
• Lifestyle and nutrient patterns clustered with deficiency — Vitamin D-deficient patients were more likely to be current smokers and had lower blood levels of other nutrients such as vitamin B12 and folate. This pattern suggests vitamin D deficiency travels with broader biological stress that affects recovery capacity.
• Inflammation and immune regulation explain delayed risk — The researchers noted that vitamin D plays a role in regulating immune signaling after infection resolves. Poor regulation increases prolonged inflammation, tissue damage, and slower repair in your lungs and blood vessels. These processes unfold over weeks and months, which aligns with the delayed rise in death risk seen in deficient patients.
Higher Vitamin D Levels Mean Fewer Everyday Infections
A study published in Advances in Integrative Medicine investigated how vitamin D levels relate to the frequency of common respiratory illnesses such as colds and flu in generally healthy adults living in Australia.5 Researchers measured blood vitamin D levels in 199 adults and compared those levels with how often participants reported respiratory illnesses over the previous year.
Only about one-third of participants had blood vitamin D levels above 30 ng/mL at the start of the study. The remaining two-thirds fell into insufficient, deficient, or severely deficient ranges. Roughly half of participants reported taking vitamin D supplements before the study, yet low levels remained common, highlighting how widespread deficiency is even among health-conscious adults.
• Lower vitamin D levels lined up with more frequent infections — Participants with the lowest vitamin D levels reported the highest number of colds and flu episodes per year. Those in the severely deficient group experienced respiratory illnesses more often than participants with higher levels. When researchers analyzed the data across groups, they found a clear inverse relationship, meaning higher vitamin D levels aligned with fewer respiratory infections.
• Supplementation changed vitamin D status quickly — Participants with low vitamin D levels were offered daily vitamin D3 supplements for three months. After that period, none of the participants remained deficient, and 85% reached levels above 30 ng/mL.
Average blood levels rose from about 18 ng/mL (46 nmol/L) to roughly 39 ng/mL (97 nmol/L), showing that deficiency is reversible within a short, defined timeframe. People who began the study with the most severe deficiency showed the greatest increases in blood vitamin D after supplementation.
• Immune cell regulation explains fewer infections — The researchers explained that vitamin D influences both your innate immune system, which acts as your body’s first line of defense, and your adaptive immune system, which fine-tunes responses over time. Adequate vitamin D improves white blood cell activity while reducing excessive inflammatory signals. This balance lowers the chance that viruses gain a foothold in the first place.
• Anti-inflammatory signaling adds another layer of protection — Vitamin D also acts as a volume control for your immune system, dialing down the release of inflammatory alarm signals (cytokines) that, when excessive, damage your own lung tissue more than the infection itself. Lower inflammation helps preserve airway tissue and prevents minor infections from escalating. Over a year, this biological effect shows up as fewer total respiratory illnesses rather than just milder ones.
How to Use Nebulized Hydrogen Peroxide to Target Upper Respiratory Infections
Optimizing vitamin D improves immune readiness from the inside out, but it doesn’t change where most respiratory infections begin. Viruses typically establish themselves first in your nose, sinuses, and upper airways — areas where vitamin D-driven immune signaling still needs time to mobilize. That gap between exposure and full immune response is where infections often gain traction.
Adding a local, early-stage airway strategy addresses that vulnerable window directly, reinforcing the surface defenses of your respiratory tract while systemic immunity does its deeper work. The approach outlined below focuses on acting locally and early, supporting your body’s own frontline defenses in the exact place viruses first take hold.
By concentrating on airway hygiene and oxygen balance at the start, this strategy is positioned as a way to slow viral activity before deeper inflammation, heavy mucus production, and prolonged recovery set in.
Hydrogen peroxide is elegantly simple — water with one extra oxygen atom — yet that single addition transforms a benign molecule into a potent viral disruptor your own immune cells already produce. When you use a properly diluted solution through a nebulizer, you’re amplifying your body’s natural defenses.
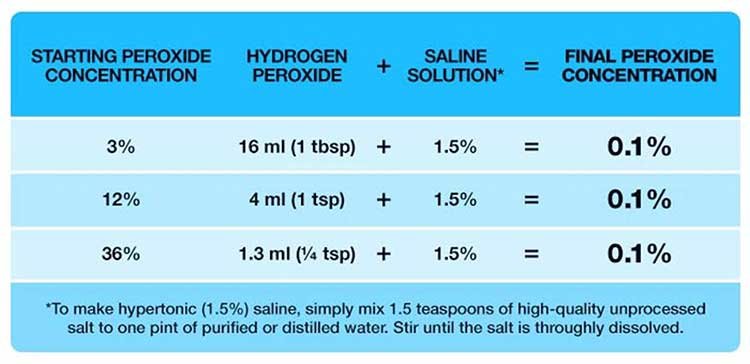
1. Target the infection directly with nebulized hydrogen peroxide — I recommend a properly diluted solution, because your immune system already uses small amounts of hydrogen peroxide to disable viruses. You amplify that natural defense by inhaling a fine mist of a 0.1% solution made from 3% food-grade peroxide diluted into hypertonic saline.
This mixture reaches your nasal passages, sinuses, and lungs where viruses replicate. If you start at the first sign of illness and repeat the sessions several times through the day, you give your airway cells the oxygen they need to shut down the virus before it spreads deeper.
2. Mix your solution correctly to avoid irritation and get full antiviral strength — Create the saline base by dissolving 1.5 teaspoons of unprocessed salt in 1 pint of distilled or purified water. You then dilute your 3% food-grade hydrogen peroxide into that saline until you reach the final 0.1% concentration.
Never use industrial-strength peroxide. Never use plain water. Your airway cells need electrolytes for comfort and safety during nebulization. If you feel stinging in your nose or throat, adjust the salt level to 0.9% by using 1 teaspoon of salt per pint. This keeps irritation low while preserving antiviral action.
3. Use a desktop nebulizer to deliver the mist exactly where the infection sits — A desktop unit gives you the fine mist that reaches deep into your bronchi and lungs. You place the mask over your nose and mouth and slowly breathe for 10 to 15 minutes. Each session uses about 1 teaspoon of the diluted mixture. If you travel often, work around crowds or feel something coming on, having a nebulizer ready gives you control when early symptoms first appear.
If you notice throat scratching or sinus pressure, use the nebulizer several times through the day. In the clinical experience of Dr. Thomas Levy and Dr. David Brownstein, respiratory symptoms begin to ease within hours when this method is used early. You interrupt the viral activity quickly enough that your body doesn’t progress into deeper inflammation or heavy mucus production.
4. Use daily preventive sessions during high-risk periods — If you’re frequently in airplanes, hospitals, schools, or indoor work environments with poor air quality, one short daily session helps maintain airway hygiene. This keeps viral load low inside your nose, throat, and lungs and supports balanced oxygen levels across your airway lining.
How to Restore Vitamin D Levels
Low vitamin D significantly increases your risk of respiratory infections by weakening the immune cells that defend your airways and lungs. When vitamin D levels drop, your body loses a key tool for fighting viruses and bacteria that cause colds, flu, and more severe respiratory illness.
This vulnerability isn’t just about supplementation — it reflects how modern life blocks sunlight exposure, overloads tissues with unstable fats that interfere with vitamin D metabolism, and disconnects daily habits from the biology your immune system depends on. The goal here is to rebuild the conditions your body uses to make and manage vitamin D correctly, so your respiratory defenses, along with your heart and energy systems, stop operating at a disadvantage.
1. Get your vitamin D from sunlight whenever possible — Your skin is designed to make vitamin D3 when exposed to natural light, and daily exposure supports bone strength, immune balance, and your liver’s ability to metabolize fat. Regular sun exposure on large skin areas like your arms, torso, and legs — without sunscreen — gives your body what it needs.
The first hint of pinkness acts as a built-in signal that you’ve had enough for that day. Sunlight also stimulates nitric oxide, which improves blood flow and lowers blood pressure, while anchoring your circadian rhythm for better sleep and daytime energy.
2. Remove seed oils before spending time in midday sunlight — If seed oils still dominate your diet — soybean, canola, sunflower, safflower, corn, or “vegetable” oil — your cell membranes remain chemically compromised, leaving both skin and heart tissue vulnerable to oxidative damage.
These oils load your tissues with linoleic acid (LA), which oxidizes under ultraviolet light, making sun damage and faster burning more likely, especially during peak hours between 10 a.m. and 4 p.m. LA also disrupts mitochondrial membranes, weakening cellular energy production and driving inflammation.
If your diet has included seed oils regularly, begin elimination now while limiting midday sun exposure until you’ve been seed-oil-free for at least six months. During this transition, rely more heavily on early morning or late afternoon sun, which provides vitamin D with less risk of burning.
3. Use vitamin D3 with the right cofactors when sunlight is limited — When sun exposure is not realistic, vitamin D3 is the form that matches what your skin produces. Pairing it with magnesium and vitamin K2 improves how efficiently your body activates and uses vitamin D, while directing calcium into bones instead of arteries.
Magnesium activates vitamin D at the cellular level, and K2 protects blood vessels and supports heart muscle strength. Using these together reduces the amount of D3 needed to maintain healthy levels and improves overall cardiovascular safety.6
4. Test and track your vitamin D instead of guessing — A simple blood test removes uncertainty. Checking your vitamin D levels twice a year shows where you start and whether your approach works. Test in late winter (February/March) when levels are lowest, and late summer (August/September) when they peak.
Use sun exposure and, if needed, vitamin D3 supplementation to reach a target range of 60 to 80 ng/mL (150 to 200 nmol/L), which supports immune balance, liver metabolism, and cellular energy production. Seeing the number rise reinforces consistency, while a drop acts as an early warning long before fatigue, infections, or heart strain appear.
5. Use movement to keep vitamin D active year-round — Physical activity sustains vitamin D metabolism during low-sunlight months by stimulating the enzymes that convert stored vitamin D into its active, usable form — particularly important from November through February in northern climates.
Research shows that even during periods of limited sun exposure, people who stay physically active maintain better vitamin D function and cardiovascular resilience.7 Treat movement as nonnegotiable, especially during darker months, to keep the system online.
FAQs About Vitamin D and Respiratory Infections
Q: Why does vitamin D deficiency increase the risk of respiratory infections?
A: Vitamin D supports immune cells that defend your airways and lungs against viruses and bacteria. When levels drop too low, those cells produce fewer antimicrobial compounds and struggle to control inflammation, allowing respiratory infections to take hold more easily and progress more severely.
Q: How low does vitamin D have to be before hospital risk rises?
A: Research shows the greatest risk occurs when blood vitamin D levels fall below about 6 ng/mL (15 nmol/L). At that range, the likelihood of hospitalization for respiratory infections such as bronchitis and pneumonia rises sharply compared with levels at or above 30 ng/mL (75 nmol/L).
Q: Does improving vitamin D status actually change outcomes after infection?
A: Yes. Higher vitamin D levels are linked to better survival after pneumonia, fewer hospitalizations, and fewer everyday respiratory infections like colds and flu. Studies show that correcting deficiency improves outcomes within months rather than years.
Q: Why do respiratory infections often start before the immune system fully responds?
A: Most viruses first settle in your nose, sinuses, and upper airways. Even with adequate vitamin D, immune signaling takes time to mobilize. That early window allows infections to gain momentum unless surface-level airway defenses are supported promptly.
Q: What combination of strategies offers the strongest protection?
A: The most effective approach combines restoring vitamin D through sunlight, proper nutrition, supportive nutrients, testing, and movement, while also addressing early-stage airway exposure using nebulized hydrogen peroxide. Supporting both systemic immune strength and local airway defenses reduces the chance that minor infections escalate into serious respiratory illness.