Welcome to another exciting day at the AACR Annual Meeting 2026! Today’s schedule includes a Plenary Session on early-onset cancers, the final Clinical Trials Plenary Session, and more. Recaps from these sessions and more will be posted throughout the day.
If you missed our previous days’ live coverage of the meeting, catch up here:
Today’s Coverage
(All times are Pacific Time.)
6:15 a.m. – More Meet-the-Expert Sessions
After yesterday’s two Meet-the-Expert Sessions, attendees will have the opportunity today to engage with another four cancer research luminaries:
- Christopher R. Flowers, MD, MS, of The University of Texas MD Anderson Cancer Center, who will discuss multidimensional approaches that aid in determining the cells of origin and other characteristics of interest for large B-cell lymphoma;
- Kurt Schalper, MD, PhD, of Yale School of Medicine, who will explore methods for preventing T cells from abetting in tumoral adaptive immune evasion;
- Daniel S.W. Tan, PhD, of the National Cancer Centre Singapore, who will examine ways to improve clinical trials’ responsiveness to understanding drug resistance; and
- Maria A. Blasco, PhD, of the Spanish National Cancer Center, who will cover the phosphorylation dynamics at play in telomere conservation and maintenance.
Each session with begin at 5 p.m. Learn more about what you can expect in AACR Annual Meeting News.
9:35 a.m. – Meet the New Editors-in-Chief of Cancer Immunology Research
In January, Elizabeth M. Jaffee, MD, FAACR, of the Sidney Kimmel Comprehensive Cancer Center, and Antoni Ribas, MD, PhD, FAACR, of the University of California, Los Angeles, were named the new editors-in-chief of the AACR journal Cancer Immunology Research.
These two former AACR Presidents are currently taking questions about their plans for the journal at the AACR Publications Booth (#3537) in the Exhibit Hall until 10:15 a.m.
One final Meet-the-Editor session will be held from 12:30 to 1:30 p.m. with Cancer Epidemiology, Biomarkers & Prevention Editor-in-Chief Elizabeth A. Platz, ScD, MPH, of the Johns Hopkins Bloomberg School of Public Health. If you miss Platz then, catch her award lecture at 5:15 p.m. in room 29 on the upper level of the convention center as the recipient of the AACR-American Cancer Society Award for Research Excellence in Cancer Epidemiology and Prevention.
11:15 a.m. – Possible Risk Timeframe for Immune Checkpoint Inhibitor Therapy
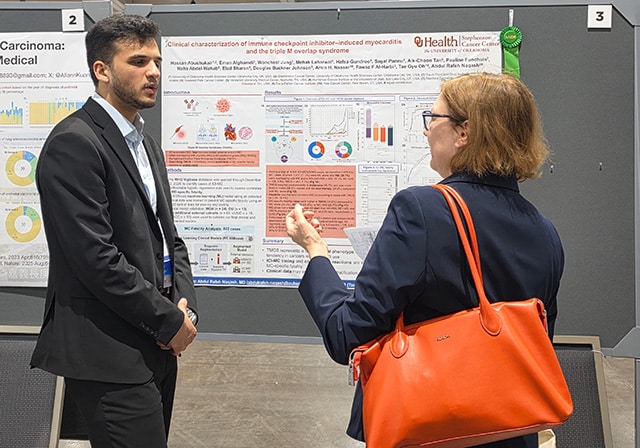
Advances in immune checkpoint inhibitor (ICI) therapy for cancer have delivered remarkable results for patients. But cancer therapy defeats its own purpose if it harms the patient more than it helps them. The study “Clinical characterization of immune checkpoint inhibitor-induced myocarditis and the triple M overlap syndrome,” presented by Hassan M. Abushukair, MD, of Oklahoma University Stephenson Cancer Center, showed that a key risk factor for patients on ICI therapy may be whether they develop myocarditis within the first month of starting therapy.
“Our analysis indicates that the first month of a patient receiving ICI therapy is the crucial period for determining patients’ risk of myocarditis fatality. If a patent on ICIs develops myocarditis in those first 30 days, that’s a flashing warning light,” said Abushukair. “This gives clinicians an actionable timeframe for determining whom ICI therapy may be dangerous for.”
In addition to highlighting the first month of ICI therapy as a possible monitoring window for myocarditis, Abushukair and colleagues also found that myocarditis-specific fatality was highest in patients with “triple M overlap syndrome”: a dangerous condition in which myocarditis, myositis, and myasthenia gravis occur simultaneously.
Abushukair hopes that the model his team is working on to predict potentially dangerous ICI responses will eventually have applications in the clinic to reduce risk.
12:20 p.m. – Bite-sized Research
Because today is the last chance to grab a bite to eat from the food trucks, we are treating you to a double serving of bite-sized research. First up, Amulya Sreekumar, PhD, from the University of Pennsylvania, who enjoyed a tuna salad sandwich as she described her work on glycan biosynthesis.
Our second serving provides a double dip of research with Long Chi Nguyen, PhD, MD, along with his mentee and cancer survivor Eva Suarez, both with the University of Chicago. As they enjoyed a little taste of Hawaii, they shared more about their work regarding tumor microenvironment-induced stress.
2:40 p.m. – Clinical Trial Results: Intralesional Nivolumab May Intercept Precancerous Oral Lesions
Injecting nivolumab (Opdivo) directly into precancerous oral lesions led to reduction in lesion size, allowed patients to avoid surgery, and preserved quality of life, according to phase I clinical trial results presented during one of today’s poster sessions.
As explained by presenter Moran Amit, MD, PhD, of The University of Texas MD Anderson Cancer Center, patients with precancerous oral lesions—which affect about 5% of the general population—often undergo surgery to remove these lesions before they progress to oral cancer, but this procedure is oftentimes debilitating. In many cases, patients can lose their ability to speak and eat after surgery.
While intravenously delivered nivolumab has shown promise against precancerous oral lesions, it comes with severe toxicities. By injecting nivolumab directly into an oral lesion, the researchers were able to deliver a much lower dose and avoid systemic toxicities. Treated lesions shrank by an average of 60% in 25 of 29 patients, and 82.13% of treated lesions continued to be cancer free twelve months after treatment.
“Our findings demonstrate that intralesional delivery of nivolumab is safe, well tolerated, and results in efficacy rates unparalleled by other nonsurgical methods, which allowed us to spare surgery for the majority of patients—spare removal of pieces of their mouth, whether it’s the tongue, the cheek, the floor of their mouth, or their palate,” said Amit.
Read the full story (in this blog post) to learn about the trial’s additional results and the experience of one of the enrolled patients.
3:30 P.M. – Clinical Trial Plenary Features New Results from Trials Testing Immunotherapy Regimens
The final Clinical Trials Plenary Session of Annual Meeting 2026, “Advances in Immunotherapy,” offered a series of updates on trials for immunotherapy.
Session Chair Ryan Sullivan, MD, of Massachusetts General Hospital, kicked things off by getting down to brass tacks. “I’m very excited for this Plenary Session,” he said, “but I’m going to stop talking now so you can hear the great science!”
Alberto Giovanni Leone, MD, of the Fondazione IRCCS Istituto Nazionale dei Tumori in Italy, presented data from the second cohort of the single-arm, nonrandomized phase II INFINITY clinical trial. The trial tested tremelimumab (Imjudo) with durvalumab (Imfinzi) as a possible organ-preservation therapy for patients with microsatellite instability-high, mismatch repair-deficient, and Epstein-Barr virus-negative gastric or gastroesophageal junction carcinoma.
After two years, none of the 17 evaluable patients had died, the clinical complete response rate was 71%, the progression-free survival (PFS) was 94.1%, and 70.6% of patients did not receive gastrectomy.
Fabrice Barlesi, MD, PhD, of Institut Gustave Roussy in France, reviewed interim results from the open-label, single-arm phase II MATISSE clinical trial, a test of the CD39-targeting antibody IPH5201 with durvalumab, plus neoadjuvant platinum chemotherapy, for non-small cell lung cancer.
Grade 3 or higher treatment-related adverse events occurred in 55% of patients, leading to nine instances of permanent discontinuation of at least one drug. One patient died of postoperative pneumonia. The pathologic complete response (pCR) rate was 27.5%.

Bruno Bockorny, MD, of Beth Israel Deaconess Medical Center, presented results on denikitug, an investigational CCR8-targeting antibody, tested in a nonrandomized, open-label phase I clinical trial for patients with advanced, treatment-nonresponsive solid tumors.
In the efficacy-evaluable population of 52 patients, the objective response rate was 8% and the disease control rate was 46%. No treatment-related adverse effects of grade 4 or 5 occurred, and the most common treatment-related adverse events were pruritic and maculopapular rash.
The last presenter, Archana Balan, MS, of the Sidney Kimmel Comprehensive Cancer Center at Johns Hopkins University, reviewed an analysis of data from the HUDSON clinical trial.
Investigating immunotherapy-resistant tumor cells identified key genomic differences between those that resisted immunotherapy from the start and those that evolved to acquire resistance. Balan identified distinct programs of genetic up- and downregulation between the populations of tumor cells with acquired and primary resistance to immunotherapy.
Additionally, cells with acquired resistance tended to display plasticity, and they were more likely to demonstrate neuroendocrine differentiation and the epithelial-to-mesenchymal phenotype—with implications for possible targeting.
4:15 P.M. – Dog of the Day

Today’s dog of the day is Gene the Lab Dog, who has big dreams of one day getting to present at the AACR Annual Meeting. Having donned the world’s tiniest lab coat, he is all ready to make discoveries of his own! If you’d like to help him start his scientific journey, stop by the AACR Shop, located outside the Sails Pavilion.
4:40 P.M. – Wildfire smoke study showed cancer risks from drifting smoke plumes
You probably know to avoid second-hand smoke if you can help it. But it’s not just cigarette haze you may want to stay away from. Being exposed to smoke from wildfires, according to the study “Wildfire smoke and cancer risk in the United States: Evidence from the PLCO Trial,” may increase the risk of developing five cancers: lung, colorectal, breast, bladder, and blood.
The study—presented by Shuguang Leng, MBBS, PhD, and Qizhen Wu, PhD, both of the University of New Mexico Comprehensive Cancer Center—used satellite images to match smoke plumes with resulting air pollution data to determine the exposures of participants in the Prostate, Lung, Colorectal, and Ovarian (PLCO) Screening Trial.
“For the general public, the key message is that wildfire smoke is not only a short-term respiratory or cardiovascular concern—chronic exposure may also carry long-term cancer risks,” said Wu. “Notably, increased cancer risk may occur even at relatively low levels of wildfire smoke [fine particulate matter] commonly experienced by general populations.”
6:40 p.m. – Special Program for High School Students
More than 90 students participated in today’s special program at the Annual Meeting for high schoolers called, “The Conquest of Cancer and the Next Generation of Cancer Researchers.” Over the course of today, the students got to interact with mentors who escorted them on a tour of the poster sessions in the Exhibit Hall, listened to lectures about cancer research and a career in this field, hear from a patient advocate about the impact of research, and even participate in a poster session of their own where they got to present their work.

For example, Selina shared her work exploring cellular diversity in chromophobe renal cell carcinoma (chRCC) using single-cell RNA sequencing. She was inspired to take up science during the COVID pandemic as she watched news stories about the need for breakthrough treatments and vigorous data analysis.
Aneesha talked about molecular profiling analyses she performed that identified signatures associated with RAS dependency. She initially wanted to get into cancer research to study the BRCA gene, but after diving into published studies, she learned that RAS mutations were associated with more cancer types and decided to switch gears.
And Rithvik discussed his study looking into how artificial intelligence could improve liquid biopsies for lung cancer detection out of a desire to see a future where tests are quick and effective.
Each of the students got a certificate for their participation and were encouraged to continue to pursue their scientific interests.
8:05 p.m. – Plenary Session Explored Potential Causes of Early-onset Cancer
This morning’s Plenary Session examined population trends and potential drivers of early-onset cancer. These cancers, commonly defined as those diagnosed before age 50, are rising in incidence, but the underlying causes are still unclear.
Hyuna Sung, PhD, from the American Cancer Society, discussed incidence and mortality trends of different cancer types across different countries. These trends highlighted the rising rates of colorectal cancer among those younger than age 50, even while incidence of this cancer has decreased among individuals age 50 and older. Sung added that analyzing trends by birth cohort, rather than by age, can reveal generational shifts in risk, identify high-risk birth cohorts, and help generate hypotheses about early-life exposures that might be drivers.
The next presenter was Andrew T. Chan, MD, MPH, of Massachusetts General Hospital, who also served as session chair. Chan’s presentation focused on colorectal cancer, the cancer type for which the phenomenon of rising early-onset incidence is most apparent.

Chan and colleagues leveraged longstanding epidemiologic cohorts, such as the Nurses’ Health Study I and II, to examine the potential contributions of obesity and metabolism, finding a role for adolescent/early adulthood and midlife adiposity in early-onset colorectal cancer risk. Additional factors identified included in utero exposures, consumption of ultraprocessed foods, and hyperinsulinemia.
Ludmil Alexandrov, PhD, of University of California, San Diego, expanded on the topic of early-life influences on cancer risk, focusing on genetic mutations that occur early in life. He and colleagues conducted whole-genome sequencing of 981 treatment-naïve colorectal tumors, including 132 early-onset cases, from 11 countries.
They identified mutational signatures associated with the bacterial toxin colibactin in early-onset tumors, and determined that these signatures were likely generated within the first five years of the patients’ lives. These findings have led Alexandrov and colleagues to hypothesize that early-life exposure to microbial products may contribute to the rising incidence of early-onset colorectal cancer. Learn more about this topic in a commentary by Alexandrov and colleagues, published in the AACR journal Cancer Discovery.
The final presenter was Pepper Schedin, PhD, of Oregon Health and Science University, who discussed early-onset breast cancer. She noted that the rates of early-onset breast cancer have risen as the average age of menarche has gone down and the age of first childbirth has gone up. And while some have postulated that the resulting longer exposure to estrogen could be contributing to rising trends in early-onset breast cancer, Schedin countered that the rising rates began decades before these changes started to take place. Therefore, she suggests that additional factors, such as environmental and bacterial exposures, diet, and physical activity, may be at play. She also noted that early-onset breast cancers that develop in the postpartum period are associated with the highest mortality, which might be due to weaning-induced liver involution that appears to promote liver metastasis.
10:55 p.m. – Forum Session Reinforced the Importance of Advocacy in Cancer Research
Cancer research is oriented toward the ultimate goal of helping patients, but delivering that progress to patients can present problems that are distinct from typical research challenges. Luckily, patient advocates are there to help.
At the Forum Session “Reducing Research Friction: How Scientists and Survivors Can Accelerate Progress,” several patient advocates offered their perspectives on how advocacy can effectuate cancer progress in tandem with researchers.
Julie Fleshman, President and CEO of the Pancreatic Cancer Action Network, opened with the story of her father, who died just four months following an out-of-the-blue pancreatic cancer diagnosis. “I was mad,” she said, noting that at the time, there was very little progress being made against pancreatic cancer.
But since then, progress has brought the five-year relative survival rate up from 4% to 13%, Fleshman said, and she plotted the increase of pancreatic cancer survival rates alongside a corresponding increase of federal research funding dedicated to the disease.
The centrality of research funding to progress, she emphasized, was nearly impossible to overstate—with advocates being central, in turn, to maintaining continued investment in research. She also highlighted the Pancreatic Cancer Action Network’s patient upskilling program: Research Advocacy Training and Support, which gives them a crash course in the biology, data analysis, and other key concepts to give them the tools they need to more fully understand and better contribute to the cancer research enterprise.
Sharon Rivera Sanchez, CEO and founder of Trials of Color, illustrated the problem of underserved populations with what she called “the 37-day price”: the story of Clarence Hannon, a resident of Petersburg, Virginia, who passed away 37 days after a diagnosis of colorectal cancer. He’d never had a colonoscopy. Hannon was also Rivera Sanchez’s brother.
As a predominantly African American community, Petersburg, said Rivera Sanchez, is an apt example of an area where cancer research and its findings fail to reach underserved populations. She proffered the “trusted messenger model” as one intervention that could overcome the problem of health messaging falling flat. Raising awareness, she said, is good—but it can be much more effective when raised by a trusted person or community.
Anjee Davis, CEO of Fight Colorectal Cancer, spoke to the fact that patient voices can tangibly speed up progress and save money in addition to informing approaches. Illustrating this point, she reviewed an economic modeling study that suggested that a single 90-day delay in a clinical trial as a result of an amended protocol may cost as much as $140,000 in a phase II trial or up to $500,000 in a phase III clinical trial. Integrating patients into the research process earlier, she said, can provide substantial savings on that front alone.
11 p.m. – The Role of Tumor-secreted Factors and the Tumor Microenvironment in Cancer Progression and Metastasis
During a Major Symposium on “Tumor-secreted Factors: The Next Hallmark of Cancer?” presenters shared cutting-edge insights into interactions and selective vulnerabilities in the tumor microenvironment, highlighting how these aspects of cancer biology are opening new avenues for innovative therapeutic strategies.
“What we’re hoping you will take away from this session is that no tumor is an island,” said Session Chair Ashani T. Weeraratna, PhD, of Johns Hopkins University, emphasizing the interactive nature of tumors with the surrounding environment, and that to effectively treat cancer, investigators need to take cohesive and comprehensive approaches that involve the tumor microenvironment.
During the first presentation, Rushika M. Perera, PhD, of University of California, San Francisco, discussed her research on lysosome-mediated cellular adaptation in primary and metastatic pancreatic cancer, which is characterized by upregulation of the autophagy and micropinocytosis pathways, both related to protein degradation. As a consequence, lysosomal biogenesis is dialed up to support the increased flux of traffic that comes to the lysosomes to be degraded.
Perera’s team isolated lysosomes from tumors grown in vivo by seeding pancreatic cancer cells in the pancreas of mice, representing primary tumors, and in the lung and liver of the same mice, representing metastasis. They then used proteomics to analyze the resident and cargo proteins within the organelles. Through this approach the researchers found that an enzyme called legumain (LGMN) was more prominent in lysosomes isolated from the metastatic sites than in those isolated from the pancreas. A similar pattern was also observed in patient-derived tissues.

Through functional and in vivo studies, the team found that loss of LGMN leads to accumulation of immature, single-chain cathepsins, which are then secreted into the extracellular space, where they mediate the breakdown of extracellular matrix proteins like collagen. Reduced collagen within the microenvironment results in failure to establish an appropriate niche and impaired tumor growth in the liver. These findings revealed that LGMN is selectively required for growth of cancer cells in the liver and may represent a potential target for the disruption of the metastatic niche.
Jeevisha Bajaj, PhD, of University of Rochester, discussed the role of the microenvironment in the context of leukemia, elucidating some temporal changes in composition of the leukemic microenvironment and how the bone marrow niche and secreted metabolites support acute myeloid leukemia (AML) growth. Using single‑cell transcriptomics and functional genetic models, Bajaj and team showed that taurine produced by cells of the osteolineage in the bone marrow supports AML growth by regulating glycolysis and mTOR signaling in leukemic cells. The researchers found that expression of CDO1, which promotes the production of taurine, increases with disease progression; that blocking taurine production in osteolineage cells impairs leukemia progression; and that inhibition of the taurine transporter SLC6A6 blocks AML growth in vivo. These findings helped establish taurine uptake as a microenvironment-related dependency in AML.
Closing the session, Weeraratna presented her lab’s work on the role of the tumor microenvironment in melanoma as it relates to aging, with focus on stromal fibroblasts, the factors they secrete, and how those impact the signaling within tumor cells and the biophysical matrix in which they reside.
Weeraratna and colleagues found that melanoma takes much longer to metastasize in young patients than in older patients, due to dormancy. Weeraratna compared tumor dormancy to the tale of Sleeping Beauty, who slept for 100 years covered by a protective hedge of thorns; dormant tumor cells, she said, do something similar sitting in a protective matrix secreted by fibroblasts and kept in check by the “enchanted spells that are immune cells.” The team unveiled that secreted factors during aging serve as the prince’s kiss to awaken dormant cells. These factors, produced by fibroblasts in response to tumor cells in the microenvironment, include immunosuppressive molecules and promote migration of myeloid-derived suppressor cells. Weeraratna also discussed the lab’s latest research on aging and the tumor microenvironment in melanoma brain metastasis.
Thanks for reading today’s updates! If you made it through all of these today, then make like Sleeping Beauty and go to sleep.